Children with Spinal Muscular Atrophy Have Poor Bone Health, Study Finds
Written by |
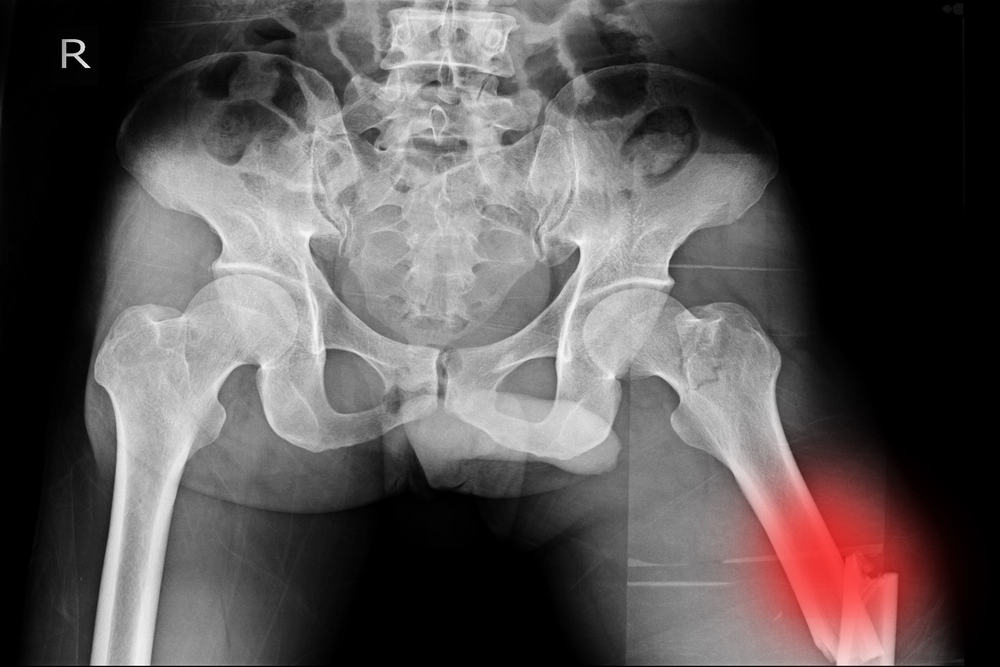
Children with spinal muscular atrophy (SMA) have poor bone health that leads to common thigh-bone fractures, regardless of the state of their disease, according to a study.
Although few of the children could be classified as having osteoporosis, researchers noted that osteoporosis criteria were developed for healthy children. That means the criteria may not capture the real state of poor bone health in SMA patients. So there could be an underestimation of bone disease in the young patients, the researchers said.
Poor bone health in SMA is still too poorly understood to design effective interventions, the researchers added.
The study, “Low bone mineral density and fractures are highly prevalent in pediatric patients with spinal muscular atrophy regardless of disease severity,” was published in the journal Neuromuscular Disorders.
Researchers at Cincinnati Children’s Hospital Medical Center reviewed the medical records of 85 children with SMA type 1, 2, and 3. They discovered that the vast majority of patients, 85 percent, had bone mineral density scores lower than normal.
Low bone mineral density was detected throughout the skeleton in children with SMA type 1. Type 2 patients had low density mostly in the lower spine and parts of the thigh bone. Type 3 SMA children were affected only in thigh bones.
Thirty-eight percent of the entire group had at least one fracture. SMA type 1 patients were at numerically greater risk of a fracture, but the difference was not statistically significant. They did, however, get their first fracture at a younger age.
Only 12.9 percent of the children were judged to have osteoporosis — a stark difference to the measures of low bone mineral density and high rates of fractures.
Fracture of the thigh bone, or femur, accounted for 44 percent of all fractures — 25 of 57 — and was the most common fracture location in all SMA types.
Children with SMA are known to have poor bone health. One reason is that strong bones develop only when exposed to weight-bearing activity during growth. In addition, research shows that the SMN protein directly interacts with bone cells, contributing to poor bone health in SMA patients.
To better understand how the decline of bone mineral density develops over time in different types of SMA — knowledge that would allow doctors to design of interventions to prevent fractures — the research team suggested that much more work is needed.
“Fracture risk is high for children with SMA,” the authors wrote. “Importantly, more work is needed to identify effective interventions to delay the decline in BMD [bone mineral density] and prevent fractures in children with SMA.”



