Mutations That Cause SMA May Also Protect Against Infection, Hinting at Why They Continue to Thrive
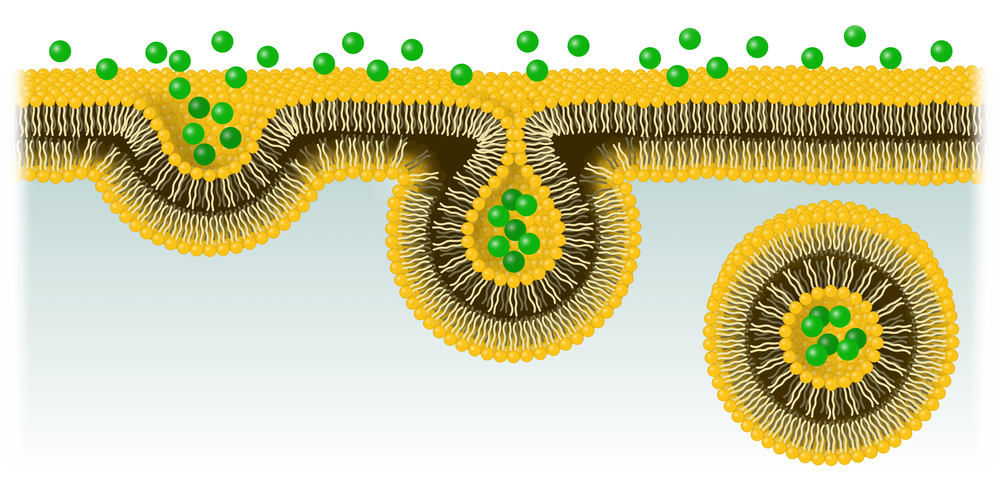
Diminished levels of the survival of motor neuron (SMN) protein causes spinal muscular atrophy (SMA), and also disrupts a process called endocytosis — crucial for the transfer of nerve signals between cells.
The findings, published in the journal PNAS in the study, “Decreased function of survival motor neuron protein impairs endocytic pathways,” at the same time, help to explain why a gene, SMN1, with such devastating consequences has continued to thrive. The process of endocytosis also allows viruses to infect cells, and a defect in the mechanism could protect people from infection.
Even though researchers have known for long that the lack of SMN makes neurons in the spinal cord die, they have not been able to figure out exactly how that happens. Researchers at Brown University in Rhode Island used both the flatworm C. elegans and human cells to get a closer look at SMN molecular processes.
During their work, they discovered that a lack of the protein disrupts endocytosis — a process whereby cells transport molecules from the outside to the inside of the cell by engulfing the molecule in a part of the cell membrane. Imagine reversing the process, whereby bubbles float to the surface and burst in your carbonated drink, and you’ll have a rather close depiction of what endocytosis is about.
In your soda, the bubbles transport carbonic acid, but in nerve cells, such bubbles are crucial for transporting neurotransmitters back into the nerve cell for recycling once a nerve has released a signal.
“Without this specialized neurotransmitter recycling and endocytosis, synaptic vesicles are not recycled fast enough to keep up with nerve and muscle cell activity,” said Anne Hart, a professor of neuroscience at Brown, in a news release.
The process is, however, not limited to neurons. Viruses, as well as certain bacteria, hijack this cellular function to infect cells. Studying the interactions with a virus and human cells from both healthy individuals and SMA patients, the research team noted that the virus could not infect cells as effectively when the endocytosis process was disrupted.
Usually, harmful genes, particularly those causing death at young ages, are lost through evolution, since sick individuals are unlikely to survive long enough to have children. But In Caucasians, there is one carrier of a mutated SMN gene for every 40 to 50 people, making it rather common.
This strange circumstance can now be explained — carriers of the gene are protected from infection, giving them a survival advantage.
“It seems possible that SMA is relatively common because carriers might be protected from infection,” said Dr. Hart. “If carriers are more likely to survive and reproduce, then evolutionary pressure might favor carriers in the long term, as is seen for sickle cell anemia and malaria infection.”
Dr. Hart, however, underscored that the study does not really prove that SMN carriers get sick less often, because such a notion would need to be further explored. “But no one has even considered this idea before,” said Dr. Hart. “Here we have preliminary results suggesting this novel idea could be true. In the world of infectious disease genetics, we hope that SMN is now on the radar.”
Another facet that the study did not explore was how the lack of SMN disrupts endocytosis. Dr. Hart and her team are now looking toward that horizon.







